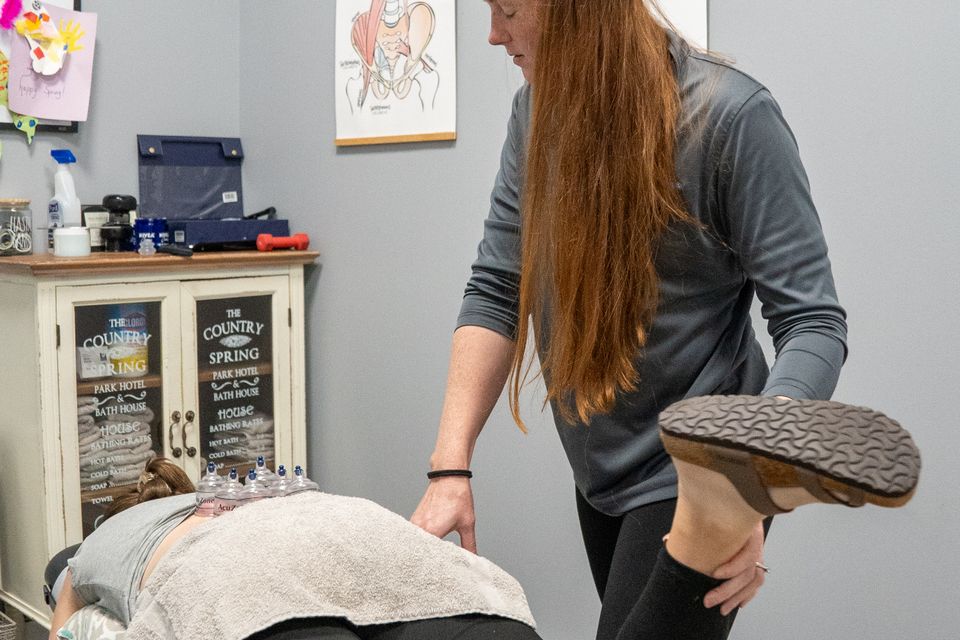
From a sports chiropractic and physical therapy perspective, this distinction is critical. Why? Because the treatment approach for true sciatica versus pseudo-sciatica is not the same.
If a patient is dealing with genuine nerve root compression, care may involve strategies aimed at reducing pressure on the nerve—such as spinal decompression techniques, specific directional exercises, and careful activity modification. These cases also require close monitoring for progressive neurological symptoms.
On the other hand, if the root cause is muscular tightness, joint restriction, or faulty movement patterns, the focus shifts. Treatment may include soft tissue therapy, joint mobilization or manipulation, corrective exercise, and neuromuscular re-education. Strengthening weak areas, improving mobility where needed, and retraining proper movement can often resolve symptoms effectively and prevent recurrence.
This is why a thorough evaluation is so important. At our clinic, we don’t just rely on symptom descriptions—we assess movement, strength, flexibility, nerve function, and overall biomechanics to identify the true source of the problem. Two patients may both report “sciatica,” but require completely different treatment plans to get better.
The takeaway is simple but important: not all leg pain is true sciatica. Self-diagnosing based on internet searches or generalized advice can lead to frustration and delayed recovery. If you’re experiencing radiating pain, numbness, or discomfort in your back or leg, getting an accurate diagnosis is the first step toward effective treatment.
When you understand the “why” behind your symptoms, you can take the right steps to not only relieve pain—but to move better, perform stronger, and reduce the risk of it coming back.